Background
Osteoporosis - brittle bones - is a disease that weakens bone strength. All people lose bone mass or tissue as they age, but the speed of the process differs. This PhD project aims to develop a telemedicine solution that can make hip-fracture patients live independently and self-reliantly in their own homes.
40.8% of all women and 17.7% of all men over the age of 50 have osteoporosis, corresponding to 537,940 Danes.
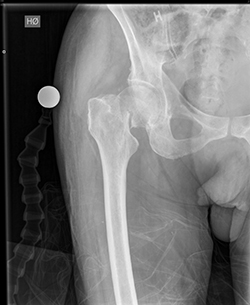
The project's focus group is patients, who are hospitalised and treated for osteoporotic hip fractures, as hip fracture is the most common cause of hospitalisation in a department of orthopaedic surgery.
When patients are discharged after accelerated courses, what do they need in order to cope with their current situation? How can we ensure their safety in connection with the discharge? How can we support their activeness when treated in their own home, where much is left to the patients themselves? Which telemedicine solution can substantiate this process - also in terms of preventing future fractures?
The reason for the topicality of this study is a steady increase in the number of age-adjusted incidences of osteoporotic fractures - mainly because of the growth in the elderly population. At the same time there are clear indications that patients want and need to be involved in their own treatment. Use of technology has already proven to be an effective tool to support communication and cooperation between citizens, patients and health professionals with the result that patients' self-care has been improved and admissions and unnecessary contacts with the hospital have been prevented.
The costs associated with osteoporotic fractures are high - for the patients in terms of functional decline and pain - for the families - and for society's health economics. A man with osteoporosis costs on average 540,000 DKK and a woman 520,000 DKK all inclusive. The study shows that the total estimated cost of osteoporotic fractures in Denmark amounted to 1.563 billion EUR in 2011. The most expensive fractures were hip fractures, man and woman alike. Approximately 30% of patients, who have experienced a hip fracture, are dependent on help from others. At the same time reports on prevention, safety and consistency in patients with hip fractures show that all the interviewed patients have had a number of fall accidents before they were hospitalised with fractures, but none of the patients see themselves as "persons who fall." This provides a special challenge in terms of preventive actions, since such patients will not be inclined to accept solutions that contradict their self-concept. The study uses Participatory Design as an overall approach method. As the name suggests, participation is highly weighted - i.e. the involvement of and cooperation with users when developing, using , and evaluating new ways of communication and organisation with the aim of introducing health services by means of technology. Participatory Design (hereinafter PD) has roots in action research but with a technological and organisational starting point. PD has gained ground in health-related research over the past 6-8 years.
Vision and Purpose
The project focuses primarily on identifying the patients' needs: what makes the patients feel safe in connection with the discharge for hip fracture and what can support and strengthen their self-care, activeness and empowerment in the time following a hip-fracture surgery. Secondly, the objective is to design, develop and test, in cooperation with all stakeholders, a health-technology solution that can satisfy such needs.
Expected Results
Denmark is in the midst of a restructuring of its health service to be completed when the new hospitals are ready to open their doors within the next 5-10 years. The design and size of the new hospitals are based on the assumption that 70-80% of all emergency patients will get the required treatment in the new emergency reception areas. It is also expected that the average length of a hospital stay will be reduced by approximately 34% which altogether will lead to a reduction in the number of hospital beds required by approximately 20% when compared to today's average. However, the short stays in hospitals will probably put more pressure on other health-care providers, like municipalities, GPs, rehabilitation teams etc. It is also likely to put pressure on the patients' own network - especially their relatives.
The design of this project provides for the development of medical technology in close cooperation with the users (patients, relatives and health professionals from the primary and secondary sectors). At the end of the project, the technology solutions developed will be instrumental in optimising the use of the services offered by the health-care sector and in strengthening the patients' own participation and motivation to take responsibility for their own health after a fracture caused by osteoporosis - but also in relation to the prevention of future fractures. The design provides for continuous cross-sectoral implementation. Thus, the challenges typically seen in relation to the implementation of new technology will be solved along the way and in close cooperation with users and organisations involved in health care.